Request
for an appointment
What is plantar fasciitis?
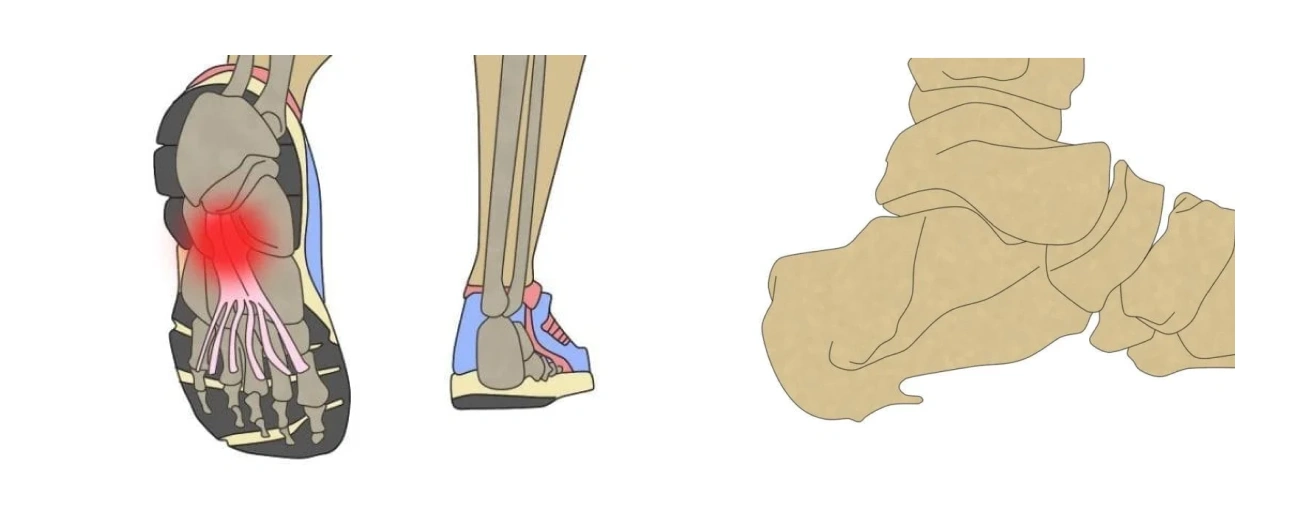
The plantar fascia is a fibrous band of elastic tissue that runs along the sole of the foot from the heel to the metatarsal area. Plantar fasciitis is the inflammation of this wide, thick band of tissue, known as fascia or aponeurosis, located on the sole of the foot.
An overload in this area of the foot produces inflammation and pain in the anteriomedial part of the heel. This inflammation does not present itself acutely, but begins gradually. The pain usually occurs with the first steps in the morning, and becomes more acute after physical exercise rather than during exercise.
The plantar fascia has an important biomechanical function during walking. Together with other structures of the foot, it is responsible for maintaining the arch or plantar vault, cushioning the impact of the foot against the ground when walking, as well as protecting the metatarsal area.
Is plantar fasciitis a common problem?
Plantar fasciitis is seen in adults of all ages but mainly in women between the fourth and sixth decade of life. Recent studies show that up to 1 in 10 people suffer from this problem at some point in their lives.
This condition must be treated in time, otherwise it can become chronic, affecting your daily activities and contributing to the development of other problems in knees, hips and spine.
It is a very frequent pathology, mainly in young non-active people who start a physical activity or simply in active people who increase their usual activity.
What symptoms may lead us to suspect plantar fasciitis?
An overload in this area of the foot, produces inflammation and pain in the anteriomedial part of the heel (in the insertion zone of the plantar fascia). This pain is more intense in the morning when we get out of bed or after being seated for a period of time. The reason is that when we rest the fascia is at rest and when the first steps are taken, a stronger traction is generated and after a while walking it stretches and the discomfort is not so noticeable.
However, the pain may also worsen throughout the day.
In the early stage of plantar fasciitis in athletes, the pain will occur in the morning or after exercise. If not treated properly, fasciitis can worsen and become chronic to the point of limiting a person’s daily life.
What is the difference between fasciitis and heel spurs?
The main difference is the presence of a calcaneal spur. The spur is a calcification that occurs at the level of the heel bone or calcaneus and requires specific treatments. This calcification is caused by excessive and repeated stretching that causes microtrauma to the plantar fascia. .
When a simple lateral calcaneal x-ray shows calcification, we speak of a spur, and when there is no calcification, we speak of plantar fasciitis. The symptoms and treatments of both have the same objective, to reduce the tension of the plantar fascia, reducing inflammation in the area and eliminating pain.
Therefore, early diagnosis is important to reduce plantar fascia tension as soon as possible and prevent it from becoming chronic.
In which sex is plantar fasciitis more frequent?
Women who do not play sports on a regular basis and patients with spondyloarthropathies have a higher prevalence of plantar fasciitis. However, in the population that practices sports, the prevalence is similar between both sexes.
When talking about fasciitis in women, there is a relationship between the length of the posterior leg musculature and plantar fasciitis. Wearing high-heeled shoes causes progressive shortening of the posterior leg musculature and increases the likelihood of developing plantar fasciitis.
Women who suffer from recurrent plantar fasciitis and wear high-heeled shoes should remember that it is important to gradually reduce the height of the shoe to avoid a sudden change that could cause tendinitis of the Achilles tendon and even back pain.
Are there any new therapies to treat plantar fasciitis?
The least invasive treatment with the best overall results is custom orthotics to offload the plantar fascia.
In addition, your doctor may prescribe medication to reduce pain and inflammation. This medication may include NSAIDs (non-steroidal anti-inflammatory drugs) that help improve pain and reduce inflammation of the sole of the foot.
When fasciitis pain is acute and does not improve with NSAIDs, the foot specialist or your physician may administer a steroid infiltration into the plantar area of maximum pain.
When medication, rest and local cold fail to control symptoms, strengthening and stretching exercises of the plantar fascia, Achilles tendon and posterior leg musculature may be necessary. Contrast baths (hot/cold), massage and ultrasound help with long-term recovery.
When plantar fasciitis becomes chronic and does not improve with the treatments described above, surgery may be necessary.
It is important to remember that shock wave treatments have been shown to be painful with mixed results.
How to treat plantar fasciitis?
The greatest difficulty in resolving fasciitis definitively is to focus on evaluating the etiology or origin of the problem.
Inflammation of the fascia causes pain but this inflammation is produced by increased stress on the plantar fascia due to, for example, the type of foot, the shape of the footprint, musculoskeletal alterations, etc.
When only the acute phase of fasciitis is treated, the inflammation is reduced and the patient improves temporarily until it recurs again because the increased stress on the fascia has not been reduced.
Plantar fascia stretches
It involves leaning the body forward, placing one affected leg behind, so that the leg and toes are in extension. The front knee should be flexed and, at the same time, keep the back leg straight with the heel firmly supported, this produces the forced extension of the plantar fascia of the affected foot. This produces the stretching of the plantar arch (plantar fascia). It should be kept stretched and perform 10 repetitions of 10 seconds each. The best time to perform these exercises is usually first thing in the morning or at the end of the day.
In the San Roman Medical Podiatric Clinic we recommend stretching exercises of the fascia before and after exercise. When these stretching exercises are insufficient, at the San Roman Clinic we perform a computerized study of the gait, for the subsequent development of orthopedic insoles under plaster cast.
Request your appointment now using our contact form or by calling us by phone, we will be happy to answer your questions.
What is the usual treatment for plantar fasciitis?
When a patient presents with initial symptoms of plantar fasciitis, the first thing to do is to rest the foot and medication prescribed by a physician to reduce the inflammation. It can also be combined with physiotherapy exercises.
The next step is to see a foot specialist for a gait study to assess the distribution of pressures and their relationship to the presenting symptoms. The results of the study will help in the preparation of an orthopedic insole under a plaster cast. This custom-made insole reduces stress on the plantar fascia, eliminating inflammation and pain. Once the plantar fascia stops hurting, it is important to start physical activity gradually with appropriate footwear for each activity.
It is important to note that there are now a multitude of “gait studies” but not all offer the same thing. The studies carried out in sports stores are designed exclusively to advise on the type of shoe and therefore do not serve to treat fasciitis or other problems.
Medical treatment with anti-inflammatory drugs
Anti-inflammatory drugs have an analgesic and anti-inflammatory effect that helps reduce inflammation and pain in the sole of the foot. These medications can be Ibuprofen or Diclofenac among others.
You should always consult your doctor and read the package insert before taking any medication. If you have no contraindications, you can take them daily for two weeks according to the indication prescribed by your doctor, and if symptoms persist, you should consult again.
These drugs should be administered with meals.
Orthopedic insoles
There is a wide variety of standard insoles on the market that offer a small amount of support and comfort. However, the insoles must be adapted to the individual needs of each foot, for this it is necessary to perform a gait study and examination of the footprint by a health professional.
FAQ – Frequently Asked Questions
Can plantar fasciitis recur?
When only the inflammation of the plantar fascia is treated without correcting or reducing the excess stress on it, the problem recurs and becomes chronic. Chronic plantar fasciitis is also much more difficult to resolve.
Does the type of footprint have an influence on being more prone to plantar fasciitis?
The shape of the foot and the way it is stepped are the main cause for developing plantar fasciitis. The types of feet that we are going to find are cavus and valgus feet. . In both cases, there is a decrease in the support of the external lateral area, leaving the fascia in a position of increased tension that with time and exercise becomes inflamed and causes pain.
The best care in foot surgery and podiatry
Clínica San Román combines experience with the latest technology to offer you the highest quality treatments in podiatry and foot surgery.
